Does Stretching Actually Benefit Us? The idea that we should stretch our muscles before…
Sciatica

Sciatica refers to pain that radiates anywhere along the path of the sciatic nerve. Sciatica is a term used to describe a symptom and is not a set pathology.
The sciatic nerve originates from the sacral plexus which is essentially a branching network of intersecting nerves, in this case found at the base of the spine.
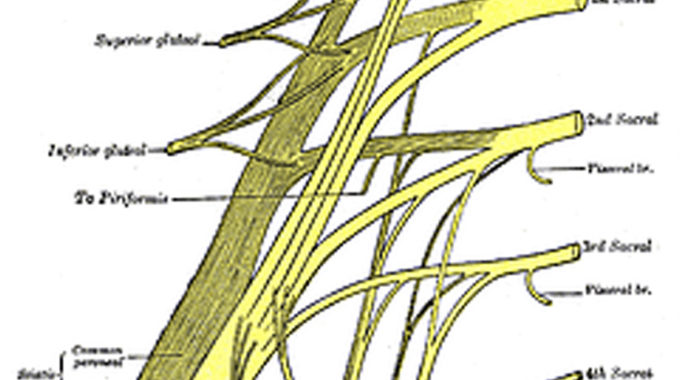
The Sciatic nerve is divided at its roots into 5 segments, separated by vertebrae, from the 4th lumbar to the 5th Sacral Vertebrae before forming one nerve (See Pic 1)
(Pic 1)- Nerve roots!

What does sciatica feel like?
People often describe Sciatica as:
Shooting pain,
Stabbing,
Dull ache often described as “toothache”
Crawling sensations “like ants”
Burning
Pins and needles
Numbness
Sciatica can affect both sensation and muscle strength so you may experience weakness as well (I will discuss this more later on).
The exact location of the pain and/or weakness depends on where exactly the sciatic nerve is being irritated.
The factors that aggravate your pain (such as bending, walking, twisting etc) depend on what has caused the sciatica, i.e. what structure/structures are involved, as they behave in very different ways.
A bit of Anatomy (not too much)
Where Does the Sciatic Nerve go?
The sciatic nerve passes from either side of the lower back and extends through the buttock on either side and down into the back of the leg where it splits into the Tibial Nerve and the Common Peroneal Nerve. (Pic 2)
The Tibial and the Common Peroneal Nerves both further divide into additional sensory and motor nerves, supplying different sections of our lower limb with sensation and muscle stimulation.
(Pic 2)- Sciatic nerve dividing

Sciatica is a fairly vague term used to describe irritation at some point along the sciatic nerve, however for the purposes of this article we are going to focus on the lower back otherwise you will be reading this all day.
If the irritation is in the lower back, the referred leg pain location can provide a very useful guide to knowing more accurately what the cause may be.
Regarding location of pain, the different nerve roots (L4-S3) provide the sensation to the skin in different areas of the leg which we can use like a map. Areas of skin supplied by a single spinal nerve root are called dermatomes. (See Pic 3)
(Pic 3)- Sensory Chart (Dermatomes)

The pain location as in Pic 3 helps to define the location of the problem, however this is also true of muscle activation as each nerve root (Pic 1) supplies the signalling to different groups of muscles as well. (see Pic 4).
Take for example L4. This supplies the sensation to the inner portion of the calf to the front of the shin and knee and also provides the signals to the muscles that bend your ankle upwards. If you were to come into the clinic with pain in this area and a weakness in your foot that meant you struggled to lift your toes up it would point towards the area of L4 and we would delve deeper to see if this was the case.
What can cause sciatica?
Again thinking about the lower back, there are several structures that can cause sciatic pain but the most common is a disc bulge or herniation (NOT a slipped disc! as this is a rather inaccurate term due to the fact that discs do not slip).
Discs are like fibrocartilaginous cushions which sit between 2 vertebrae and provide not only shock absorbency but also anchor our vertebrae together (like a ligament), enabling us to bend and move at each spinal joint.

Discs consist of a softer gelatinous inner portion called the Nucleus and a tougher outer layer known as the annulus (picture a jam doughnut).
In the case of a disc bulge, a tear in the annulus (over time or through sudden trauma) can result in movement of the nucleus into the weakened wall which can form a bulge (similar to inflating an old inner-tube on a bike and getting a small bubble forming).
Due to its position close to the nerve root this bulge can cause compression of this root and as discussed earlier cause pain in a different are of the leg depending on the nerve root involved (Pic 3).

Disc bulges or herniation’s are often caused by a bend/twisting movement or a lift, or all combined as the pressure exerted on the disc is at its highest. The worst position for discal pressure is bending and twisting to lift an object when sat.
What can you do to minimise the chance of getting sciatica?
Posture- we live in a world where sitting takes up most of the day so making sure to sit upright and not slumping can make a big difference to spine health. This is because the structures of the spine (including the discs) are all positioned with more evenly distributed pressure. This can be helped with use of a pillow in the lower back or with a good lumbar support in your chair. Take a few minutes to make sure your desk and chair is set up correctly to enable you to do this or ask for a work station assessment if this is an option where you work. If you have any specific questions about this make sure to call your local Physio for advice.
Keep active- Again this refers to avoiding living an entirely sedentary life. If you sit slumped all day it is important to reverse this with some form of exercise that means you are standing up increasing your heart rate and getting moving (even just getting out and having a brisk walk). Core stability exercises can also help to reduce the risk as these muscles help to support the spine.
NB- Obesity and smoking has been shown to increase the likelihood of suffering from sciatic pain so losing a bit of weight and quitting smoking may indeed help.
Lifting technique- whether you are a manual labourer or just enjoy a bit of gardening it is hugely important to lift correctly, with the object in-front of you as much as possible, your back straight and knees bent so you can avoid bending and twisting of the lower back.
What if I have sciatic pain now?
Due to the nature of sciatica, it is very important that you get it assessed as soon as possible by your Physio or appropriate health care professional as finding the cause is the key to easing symptoms and helping to prevent episodes in future. Treatment often involves manual therapy to reduce muscular tension and joint stiffness as well as exercises aimed at restoring/improving core and lower limb strength and mobility.
So, sciatica is often treatable conservatively but it does require the correct management which is why my advice will always be to go to your local Physio for advice” as they will be able to discuss the best plan of action, whether that be manual therapy, exercise, postural adaptations at work etc or referral back to your GP for further investigations (MRI etc).
IMPORTANT: If you notice any of the following symptoms: Bladder or bowel disturbances which may include incontinence (inability to retain urine or stool), and/or constipation (inability to eliminate urine or stool) or numbness in your groin you need to call your GP immediately and if unable to get through go straight to A+E and tell them your symptoms. This is very rare but if a certain group of nerves called the Cauda Equina get compressed it can lead to ongoing issues with bladder/bowel if not addressed within a short time frame.
It is also very important to call your GP if you have worsening weakness or tingling/numbness!
If you have any questions about this topic or any other areas you want me to go through please call me (Luke) on 01799530650 or send me an email to reformphysio@outlook.com.
Reform Physiotherapy is a new clinic based in Little Chesterford, near Saffron Walden. Feel free to visit ‘contact’ for more details of how to find us.



